Radiation in Fracking Wastewater
January 29, 2013Alarming Questions about EPA’s Oversight of Oil and Gas Drillers
January 31, 2013Published: January 27, 2013
http://www.nytimes.com/2013/01/28/us/boom-in-north-dakota-weighs-heavily-on-health-care.html?_r=0
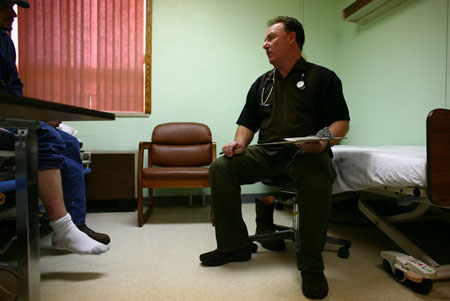
Dr. Gary Ramage treating a patient at McKenzie County Hospital in Watford City, N.D. The hospital now averages 400 emergency room visits per month. –Matthew Staver for The New York Times
WATFORD CITY, N.D. — The patients come with burns from hot water, with hands and fingers crushed by steel tongs, with injuries from chains that have whipsawed them off their feet. Ambulances carry mangled, bloodied bodies from accidents on roads packed with trucks and heavy-footed drivers.
The furious pace of oil exploration that has made North Dakota one of the healthiest economies in the country has had the opposite effect on the region’s health care providers. Swamped by uninsured laborers flocking to dangerous jobs, medical facilities in the area are sinking under skyrocketing debt, a flood of gruesome injuries and bloated business costs from the inflated economy.
The problems have been acute at McKenzie County Hospital here. Largely because of unpaid bills, the hospital’s debt has climbed more than 2,000 percent over the past four years to $1.2 million, according to Daniel Kelly, the hospital’s chief executive. Just three years ago, Mr. Kelly added, the hospital averaged 100 emergency room visits per month; last year, that average shot up to 400.
Over all, ambulance calls in the region increased by about 59 percent from 2006 to 2011, according to Thomas R. Nehring, the director of emergency medical services for the North Dakota Health Department. The number of traumatic injuries reported in the oil patch increased 200 percent from 2007 through the first half of last year, he said.
The 12 medical facilities in western North Dakota saw their combined debt rise by 46 percent over the course of the 2011 and 2012 fiscal years, according to Darrold Bertsch, the president of the state’s Rural Health Association.
Hospitals cannot simply refuse to treat people or raise their rates. Expenses at those 12 facilities increased by 15 percent, Mr. Bertsch added, and nine of them experienced operating losses. Costs are rising to hire and retain service staff members, as hospitals compete with fast food restaurants that pay wages of about $20 an hour.
“Plain and simple, those kinds of things are not sustainable,” he said.
Many of the new patients are transient men without health insurance or a permanent address in the area. In one of the biggest drivers of the hospital debt, patients give inaccurate contact information; when the time comes to collect payment, the patients cannot be found. McKenzie County Hospital has invested in new software that will help verify the information patients give on the spot.
Mr. Kelly has pushed for the state, which has a surplus of more than $1 billion, to allocate money intended for the oil region specifically to health care facilities in the area. He has also asked for the state to grant low-interest loans so hospitals can borrow money for facility improvements and for the governor to convene a task force to study health care issues in the oil patch.
Aides to Gov. Jack Dalrymple say he is taking steps to bolster medical training in the state, proposing to spend $68 million on a new medical school building at the University of North Dakota and $6 million to expand the nursing program at Lake Region State College. Mr. Dalrymple, a Republican, has also increased Medicaid financing for the state’s rural hospitals.
“Health care is certainly one of those areas that was targeted early on as we’ve seen growth out west,” said Jeffrey L. Zent, a spokesman for the governor.
Public utility numbers suggest that the population of Watford City has more than quadrupled to 6,500 over the past two years, Mr. Kelly said. In nearby Williston, considered the heart of the oil boom, the population, including temporary workers, has swelled to 25,000 to 33,000 from fewer than 15,000 in 2010, according to a study by North Dakota State University.
The huge population growth has produced new communities virtually overnight, creating logistical problems that affect the quality of medical care.
After a recent emergency call, Kelly Weathers, who has worked as a paramedic in the region for nearly 25 years, drove in circles with his team for about 15 minutes, searching for the address where they had been sent to treat a man who had hurt his back falling off a piece of equipment. But they could not find the street because a sign had not yet been erected. Eventually, a colleague of the injured man met the ambulance at the highway and escorted them to the site.
Mr. Weathers, who works for the Mountrail County Health Center in Stanley, said that in the past, “all the volunteers, they didn’t go by street signs.”
Charles Quinn, 43, of Mississippi, has been working in the region for eight months repairing 18-wheelers. He said his job has its dangers because he often works under the trucks while they are running.
“It’s all kind of dangerous,” he said of the jobs in the oil patch. “There’s a lot more accidents around you because you got more people around you working.”
The cramped housing camps where many oil workers live can add to health issues. On a recent afternoon at McKenzie County Hospital, a man limped into the emergency room complaining about a dry, red patch of skin on his leg. Dr. Gary Ramage, the hospital’s sole full-time physician, said it was a bite from a brown recluse spider, which had most likely nested under the trailer where the man lives.
Since the oil industry started growing rapidly in the region, Dr. Ramage said, he has had to treat many more sexually transmitted diseases. Chlamydia rates in McKenzie County roughly doubled from 2010 to 2011.
With little money to spend, hospitals are struggling to finance sorely needed improvements and hire additional medical providers. McKenzie, which is six decades old, is a one-story brick building and has one room for emergencies. (A makeshift second emergency room was created from one of the inpatient rooms.) In a building across the street that houses a clinic, a narrow hallway with dark carpet is crowded with file drawers lining the walls.
Hospital executives are hoping to get the local government to approve a 1-cent sales tax increase so they can build a $55 million medical facility that would triple the size of the clinic, expand the emergency room, maintain the 24-bed hospital and increase space for other outpatient services like physical therapy. They have also spent the past year trying to hire two new doctors. Recruiting medical professionals to the area has long been a problem.
“Let’s be honest,” Mr. Kelly said. “People think they have to move to Siberia if they move to North Dakota.”
But for now, Dr. Ramage, a gregarious Canadian who has worked here for 18 years, is left shouldering much of the load. Before the oil boom started a few years back, Dr. Ramage covered both the clinic and the emergency room. Now he mostly works at the clinic, while the hospital hires roving physicians to cover the emergency room. He is well known in the community, and people call him at home when they are sick. But now, he does not know many of the patients he sees.
“My work is no longer small-town work,” he said. “My work has now been transformed from that of a small family practitioner to basically an E.R. doc.”



